Duodenal switch surgery is one of the latest and most innovative metabolic and bariatric surgery procedures in the United States. It is used to treat patients classified as “morbidly obese” or those with a body mass index (BMI) of 50 and above. Patients who are at high risk of developing weight-related conditions are also recommended to undergo this procedure.
Also known as biliopancreatic diversion with duodenal switch (BPD/DS), it is a 2-part procedure starting with gastric sleeve surgery and ending with gastric bypass surgery. This procedure removes about 75 to 80% of the stomach and bypasses half of the small intestine to absorb fewer calories and fat during digestion. With decreased appetite and lower nutrient absorption, the duodenal switch procedure can significantly cause a healthy weight loss.
Who is considered for duodenal switch surgery?
In general, the duodenal switch procedure is a good option for patients with:
- a body mass index (BMI) of 50 or higher (morbid obesity)
- a BMI of 40 or higher, and have an increased risk for developing obesity-related health problems like type 2 diabetes, high blood pressure, and heart disease
Patients suffering from digestive issues, such as irritable bowel syndrome (IBS), gastroesophageal reflux disease (GERD), or Crohn’s Disease are not advised to undergo this procedure as it can aggravate their symptoms. Likewise, patients with pre-existing nutrient deficiencies, such as anemia, are not good candidates for this procedure.
In some cases, extremely overweight patients are advised to undergo this procedure in two stages: sleeve gastrectomy first, followed by gastric bypass 9 to 12 months later. It can also be done to sleeve gastrectomy patients who could not lose enough weight or those who regained weight after a year or two.
At Beltline Health, we are committed to providing all relevant information about weight loss surgery to help you determine if it is right for you. Our team of healthcare professionals is dedicated to helping you make the best decisions to achieve a sustainable weight and healthy lifestyle.
What to expect before duodenal switch surgery?
Since BPD/DS is a combination of two bariatric surgery procedures, surgeons also encourage patients to lose as much excess weight as possible before the actual surgery. This can be done by sticking to a low-calorie diet and avoiding oily foods, whole milk products, high-carb foods, and high-calorie drinks.
During your visits to your bariatric surgeon, they will recommend a special pre-surgical diet that should be followed to reduce the size of your liver. Most obese patients have accumulated plenty of fat cells in their liver, which need to be trimmed before the surgery. Having a normal-sized liver would allow the surgeon to have greater access to your stomach since it’s right next to it.
Similar to other weight loss surgeries, patients must also discontinue certain medications before the surgery, which will be explained by your bariatric surgeon depending on your pre-existing medical conditions.
What happens during duodenal switch surgery?
The biliopancreatic diversion with duodenal switch is a laparoscopic surgery that uses minimally invasive techniques and takes around three hours. It starts with the bariatric surgeon making five to six small incisions in the abdominal area. They will insert small surgical instruments and a camera into these small incisions to access the stomach area.
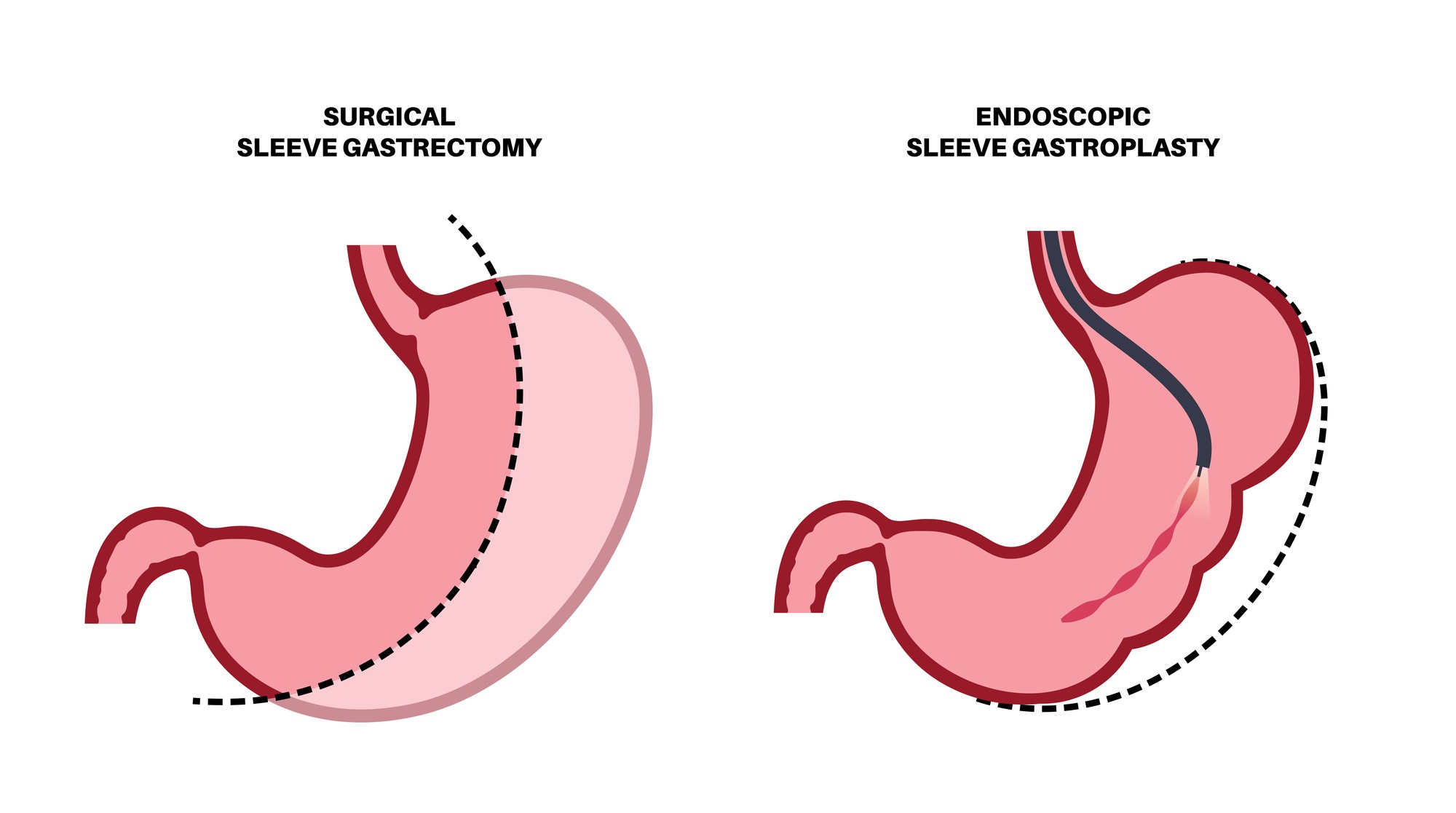
The first step is a vertical gastric sleeve surgery, where the larger portion of the stomach is removed to create a narrow sleeve in the shape of a banana. The newly created sleeve is slightly larger than when sleeve gastrectomy is performed as a stand-alone procedure.
The next and final step is similar to gastric bypass surgery. Once the portion of the stomach that releases hunger hormone is removed, the first portion of the small intestine called the duodenum is divided below the pylorus. The top portion of the duodenum is then connected to the last portion of the small intestine, where food is mixed with digestive juices. But unlike gastric bypass surgery, the duodenum is also resected, and a larger portion of the small intestine is bypassed.

What to expect after duodenal switch surgery?
Following a duodenal switch surgery, patients typically spend two nights in the hospital. Since most duodenal switch procedures are performed laparoscopically, the complication rates are relatively lower than those performed in an open manner.
Patients need to follow a special post-surgical diet of clear liquid to pureed foods during the first few weeks after the surgery. They can start to consume solid food once the new stomach is fully healed.
Since a portion of the stomach is removed and fewer nutrients are absorbed, patients need to drastically adjust their food intake and reduce portion sizes compared to pre-surgical servings.
Many patients return to their usual daily activities after two to four weeks. Fatigue is a common side effect for the first two weeks because of limited food intake, but it improves as you eat soft foods. Since nutrient absorption is significantly reduced, patients are advised to take vitamin and mineral supplements such as vitamin A, D, K, B-complex, iron, and calcium to prevent nutritional deficiencies.
Most duodenal switch patients lose around 60 to 80% of their excess weight within two years after the surgery. They must follow a highly restrictive diet that includes more vegetables, fruits, and lean proteins while avoiding simple sugars, fatty foods, and complex carbohydrates.
It takes around three months for patients to recover from duodenal switch surgery. During recovery, they are encouraged to attend periodic check-ups and progress monitoring until they reach their ideal weight.
What are the advantages of duodenal switch surgery?
Duodenal switch (BPD/DS) is a complex weight loss surgery that shows results of almost 70% of lost excess weight for over ten years. Since it is done laparoscopically, it usually results in faster healing time and fewer post-surgery complications.
Other advantages are:
- has the highest chance of losing more weight and preventing weight regain
- has the highest chance of controlling diabetes among other weight loss procedures
- has the lowest rate of weight regain among bariatric procedures
- removes the gland that secretes the hunger hormones
- reduced the amount of fat absorbed by the body
- does not require placing a foreign object inside the body
- low risk for “dumping syndrome” (rapid gastric emptying)
- the combination of restrictive and malabsorptive weight loss procedures may cause rapid weight loss
What are the disadvantages of duodenal switch surgery?
Like other weight loss procedures, BPD/DS is a non-reversible weight loss surgery since the larger portion of the stomach is removed. It also involves bypassing the small intestine, which may help patients lose weight and maintain it over the years.
Other disadvantages are:
- may worsen or cause gastric reflux and heartburn
- eating fatty foods may cause stomach cramps, diarrhea, and bowel movements
- increased risk of protein, fatty acid, nutritional deficiencies
- may develop anemia, kidney stones, osteoporosis, and fatal malnutrition because of nutrient deficiencies
Is duodenal switch surgery safe?
Duodenal switch surgery or BPD/DS is a highly complex weight loss procedure, but it is generally considered safe with proper medical guidance. It is one of the most effective and reliable long-term weight loss or weight management treatments for type 2 diabetes.
Since the procedure comes with many risks, it is crucial to work with health care professionals with extensive experience in different weight loss surgery options. At Beltline Health, our team will walk you through the detailed weight loss surgery process to determine if it is suitable for your needs.
If you’re interested in knowing more about the basics of weight loss surgery, sign up for our free weight loss seminar today. Check this article to read more about other bariatric procedures we offer.
For more information, head to our website to message us or call us at (470) 419-4380.